
empowering healthcare. improving lives
Easing the healthcare burden
Experience the impact of AI-enabled triage and automation
free up resources
Right patient, right place, right away
Healthcare services are facing unprecedented challenges with increasing patient demand combined with workforce and capacity issues.
AI-enabled triage can help to better route patients at the first point of contact - enabling busy services to free up resource and work more efficiently.
56% of incoming cases solved in one contact
market-leading AI-enabled triage
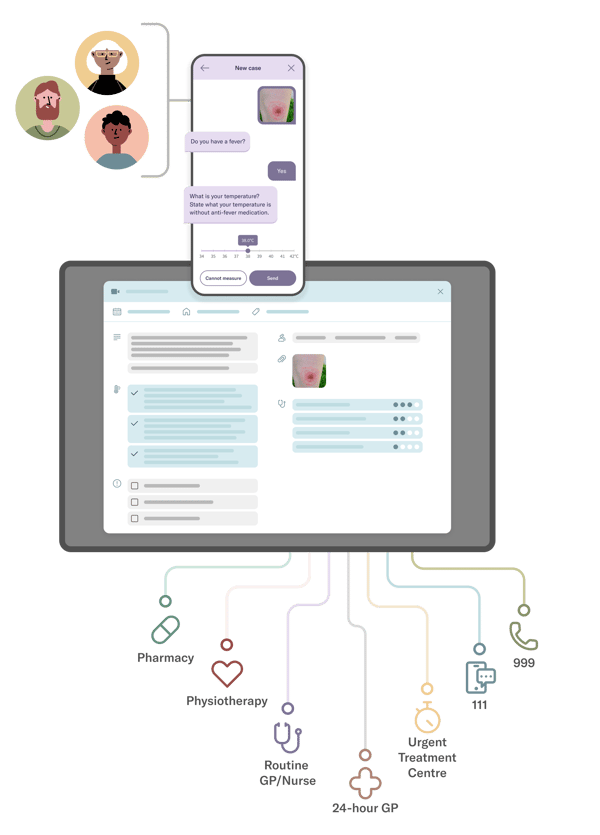
Meet Red Robin
Comprehensive patient history
Red Robin takes a comprehensive patient history for new symptoms. Continuous analysis of patient inputs means patients are asked only relevant questions.
Urgent symptoms, at any point in the questioning sequence, trigger alerts telling patients to seek urgent care.
Reliable decision support
Patient history, images, potential diagnoses and urgency can be sent to a Smart Inbox for management and allocation.
Alternatively, cases can be automatically triaged to appropriate clinics, clinicians or team members.
Respond at first contact
Armed with full details of symptoms and urgency, HCPs can respond to patients at first contact - via messaging, email, video and forms.
Routing patients to the most appropriate HCP first time, improves patient experience and enables HCPs to make the most of their time.
unique clinical feedback loop
Why we're different
Red Robin features a unique, clinically designed, end-to-end feedback loop to enable continual evaluation and refinement. 50,000 real-world clinical cases have been used so far.
Clinicians agree with Red Robin’s low acuity rating in 98% of cases
healthcare partners
Who we work with

.png?width=600&height=141&name=nhs111%20black%20logo%20(1).png)
















perspectives
Read our latest articles

Visiba appoints Dr Annabelle Painter as Chief Medical Officer to continue to drive patient safety and clinical efficiency.
Read more
Wakey Wellness – bringing health and wellbeing services to the children and young people of Wakefield
Read more